Women with incurable breast cancer have been thrown fresh hope thanks to a ‘mind-blowing’ new drug that holds the disease at bay for more than twice as long as previous treatments.
The medication can halt progression for two years, compared to just nine months with previous options, according to the latest trial results.
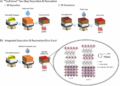
The drug, Enhertu, approved by NHS health chiefs last week, is given every three weeks in hospital via an intravenous drip, and combines two potent compounds: an antibody that helps the immune system find cancer cells and a fighter molecule, which enters the cancer cells and destroy them.

Professor Peter Schmid of the Barts Cancer Centre and a researcher involved in the development of Enhertu, said: ‘This drug is displaying mind-blowing activity in patients for whom the outcome is usually pretty poor. It is succeeding where all other treatments seem to fail, because over time, cancer cells adapt to hide from the drugs. Not only does this one work, it continues to work for a long time’

The new treatment can reduce the size of a fatal tumor stabilising it for up to two years
This two-pronged attack leads to dramatic tumour shrinkage in two-thirds of patients given it, compared to just a third having standard treatment, according to the latest trial results.
‘This drug is displaying mind-blowing activity in patients for whom the outcome is usually pretty poor,’ says Peter Schmid, professor of cancer medicine at the Barts Cancer Centre and one of the researchers of the drug.
‘It is succeeding where all other treatments seem to fail, because over time, cancer cells adapt to hide from the drugs. Not only does this one work, it continues to work for a long time.’
About 55,000 Britons are diagnosed with breast cancer every year, mostly women aged over 50. Treatments mean the outlook for most patients is positive, with more than three-quarters of women surviving at least ten years after diagnosis.
But one in five patients have a type of breast cancer that produces excess amounts of a protein involved in cell growth, called HER2. These tumours are three times as likely to spread to other parts of the body, compared with other tumours.
In up to a fifth of HER2 positive (written HER2+) patients, even if the cancer is initially eradicated, tumours recur – either in the breast or elsewhere in the body.
There are drugs and other treatments for these patients but the effects are short-lived and many run out of options within a few months. They will now be offered Enhertu, which can continue to shrink tumours for an average of 16 months.
In studies, some tumours kept reducing in size for two years during treatment.
‘These patients currently have a very limited prognosis,’ says Prof Schmid. ‘At this stage, they rarely survive longer than a year to 15 months. But now, if we have a drug that can control the disease for two years, we imagine it will significantly extend survival, too.’
Side effects occur at a similar rate to existing treatments, with roughly a third of the test patients experiencing complications such as lung infections. Experts say the most common side effects, such as nausea, fatigue and vomiting, are far less severe than seen with chemotherapy.
Enhertu is said to have a unique ability to draw the active compounds directly into the nucleus of the cancer cell, which contains its DNA, to destroy it This also minimises the impact of the drug on surrounding, healthy cells, reducing the severity of side effects. Prof Schmid says the drug could soon be licensed for use earlier on in treatment of HER2+ breast cancer – not just when patients have run out of all other options.

Enhertu, approved by NHS health chiefs last week, is given every three weeks in hospital via an intravenous drip, and combines two potent compounds: an antibody that helps the immune system find cancer cells and a fighter molecule, which enters the cancer cells and destroy them
One breast cancer patient to benefit is Alia Brown, a 32-year-old veterinary nurse from South London, who, in April 2018, developed secondary tumours in her liver. Doctors prescribed the drug Kadcyla and a heat energy treatment to destroy the liver tumours. But 16 months later, the cancers began to grow again.
‘The only option I had was to take a chemotherapy tablet, which would give me just six months of stability,’ says Alia. ‘I also knew that, if I took it once, I couldn’t take it again because cancer cells develop an immunity.’
She enrolled on the Enhertu trial last February, and admits: ‘I had nausea, fatigue and weight loss for about four months. I’m not going to lie – that was hard.
‘But almost immediately my tumours started shrinking. After about three months they stopped shrinking but were stable. Then, four months later, they started shrinking again. It was amazing.’
Last week – after 14 months on the drug – scans showed signs of growth again.
‘At this stage, you worry about not having much time left,’ she says. ‘And this drug has given me a year and two months that I otherwise wouldn’t have had.
‘Although it was difficult to start with, I missed out on the horrible chemo symptoms which are far worse. I feel so grateful to have had the opportunity, and it’s great that now thousands more will too.’