Analysis of thousands of tumours from NHS patients has identified a ‘treasure trove’ of new clues about the causes of cancer.
In the biggest study of its kind, researchers at Cambridge University Hospitals looked at the genomes of more than 12,000 people with cancer in England.
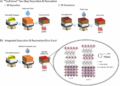
They spotted 58 new patterns in their DNA, called mutational signatures, suggesting there are causes that scientists are not yet aware of.
The researchers hope the discovery will allow future studies to work out the root of these cancer-causing mutations.
Scientists were aware of just 51 mutational signatures before the new find, including changes caused by smoking or UV light.
Identifying these signatures also allow doctors to look at each patient’s tumour and match it to specific treatments and medications.
However, the patterns can only be detected in cancer patients who have had their whole genome sequenced by scientists — which isn’t routinely done.
Professor Serena Nik-Zainal, a genomic expert who led the study, said these patterns are like ‘fingerprints at a crime scene’.
She said the findings could indicate an ‘Achilles heel’ in individual cancers that could be targeted with treatment.


Cambridge University researchers studied the genetic make-up of more than 12,000 people with cancer in England, which allows them to see the origins of the tumour. They spotted 58 new patterns in the DNA of cancer, suggesting there are causes that scientists are not yet aware of
Around 375,000 new cancer cases are diagnosed in the UK every year, while 1.7million are confirmed in the US.
Cancer is caused by mutations in the genome of cells, which causes cells to multiply out of control until they form a tumour.
The latest study, published in the journal Science, analysed the whole genome of 12,222 NHS cancer patients as part of the 100,000 Genomes Project in England.
Genome sequencing looks at all of the thousands of DNA building blocks within each tumour, showing the mutations that contribute to each person’s cancer.
Some of the new mutational patterns observed were present across many different cancer patients, while some were more rare.
Cancers are thought to have a finite amount of mutational processes, fuelling the search to identify them all and what causes them.
Knowing the signatures are present within a tumour helps to figure out the root cause of them and point towards whether the mutation was caused by environmental factors or a genetic problem.
Professor Nik-Zainal told MailOnline: ‘I sometimes use the analogy of footprints in sand where the mutational signatures are the footprints.
‘When you look across a beach, there could be footprints everywhere (analogous to cancer, mutations look a bit random, they are everywhere).
‘But if you study the footprints in detail, there are characteristics that tell you whether the footprints are an animal or a human.’
She added: ‘Mutational signatures are like those footprints. We can start to figure out whether something is due to external or cellular factors by studying the mutation patterns in detail.’
The researchers used their findings to develop an algorithm called Signature Fit Multi-Step (FitMS) that can spot mutational signatures in new cancer genome samples.
Only patients who have had their cancers whole genome sequenced will be able to benefit from this tool, but the team believes it can be rolled out to them ‘very quickly’.
As it stands, only cancers in children, specific leukaemias and sarcomas — rare cancers affecting the body’s tissues — are sequenced through the NHS but experts expect this list to be widened in the coming years.
FitMS will spot the mutational signatures in these patients’ cancer, which scientists hope will speed up the ability to match them to a more specific treatment.
Professor Nik-Zainal said: ‘The reason it is important to identify mutational signatures is because they are like fingerprints at a crime scene — they help to pinpoint cancer culprits.
‘Some mutational signatures have clinical or treatment implications — they can highlight abnormalities that may be targeted with specific drugs or may indicate a potential “Achilles heel” in individual cancers.’
Michelle Mitchell, chief executive of Cancer Research UK, said: ‘This study shows how powerful whole genome sequencing tests can be in giving clues into how the cancer may have developed, how it will behave and what treatment options would work best.’
The results can ‘potentially be used within the NHS to improve the treatment and care for people with cancer’, she added.
Professor Matt Brown, chief scientific officer of Genomics England, said applying the mutational clues to patients ‘could improve the diagnosis and management of cancer patients’.