Wearing a cloth mask may not shield the user from coronavirus because too many infected droplets can slip through, a study has claimed.
Scientists at New Mexico State University, in the US, studied five types of face coverings including cloth masks and surgical grade N95 masks.
They found that while all masks blocked at least 95 per cent of droplets from coughs and sneezes – there was still a risk of the disease being passed on.
Although cloth masks stopped 96.4 per cent of sneeze droplets at a distance of six feet, they still let more than 1,000 through – which the scientists said could carry enough virus particles to trigger an infection.
‘Wearing a mask will offer substantial, but not complete, protection to a susceptible person,’ said Dr Krishna Kota, an associate professor at the university who led the research.
The science behind mask-wearing was hazy at the start of the pandemic and authorities in the UK and other countries hesitated to recommend wearing them.
The World Health Organization did recommend masks until June 8, and then only for people over 60 and those with underlying health conditions.
In Britain, face coverings were first brought in for public transport in June, and later for shops and other indoor spaces in July. In the US regulations vary across the country, with some states setting up rules as early as April but others resisting making masks mandatory.
The general consensus now is that masks may offer only limited protection to the people wearing them, but they are quite good at stopping people spreading the disease if they have it without knowing, because they catch their breath.
Scientists have also suggested that masks could reduce severity of disease by exposing people to the virus in small doses, but this hasn’t been proven.

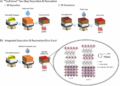
Five types of face masks were examined with results showing that the N95 (top right) blocked the most at 100% of droplets and the regular cloth mask (bottom left) blocked the least at 96.4% of droplets
‘A mask definitely helps, but if the people are very close to each other, there is still a chance of spreading or contracting the virus,’ said Dr Kota.
‘It’s not just masks that will help. It’s both the masks and distancing.’
For the study, published in the journal Physics of Fluid, the team built a machine that mimics coughs and sneezes from humans.
It uses an air generator to blow tiny liquid droplets, like those that would escape from a nose or a mouth.
The machine was tested on five different types of masks: an N95 mask, s surgical mask, a cloth mask, a two-layer cloth mask and a wet two-layer cloth mask.
The researchers say wetting a mask could help because the material’s fibers will expand, reducing the pore size accessible for droplets to get through.
Two glass square tubes were joined with a mask tightly fit between them and a camera lens to capture the number of droplets.
Each of the masks were able to block most of the droplets with the best-performing being the N95, which blocked 100 percent of droplets.
Meanwhile, the worst was the regular cloth mask, which only blocked 96.4 percent of the droplets from getting through.
However, at distances of less than six feet, letting in around three percent of droplets could be enough to make someone ill.
Studies have shown that the average infection threshold for COVID-19 is 1,000 virus particles, inhaled either all at once or on separate occasions.
In addition, a single sneeze has the potential to carry up to 200 million virus particles.
The cloth mask let through more than 1,000 sneeze droplets, each of which could have millions of virus particles.
The two-layered cloth mask with a PM2.5 filter let through more than 600 sneeze droplets.
This means that if someone wearing one of these masks is close to an infected individual, enough droplets could escape to make them contract COVID-19.
‘Without a face mask, it is almost certain that many foreign droplets will transfer to the susceptible person,’ Kota said.
‘Wearing a mask will offer substantial, but not complete, protection to a susceptible person by decreasing the number of foreign airborne sneeze and cough droplets that would otherwise enter the person without the mask.
‘Consideration must be given to minimize or avoid close face-to-face or frontal human interactions, if possible.’