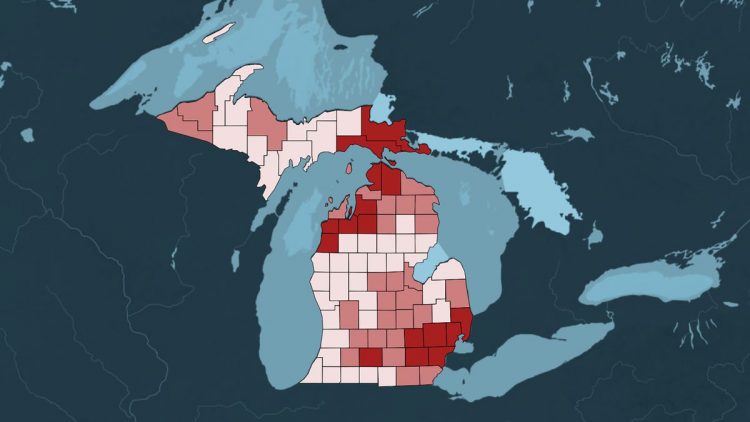
More than half of all Michiganians live in counties where they should mask up indoors following a spike in COVID-19 cases, according to recommendations from the Centers for Disease Control and Prevention.
Across the state, 16 counties — including Wayne, Oakland, Macomb and many others near heavily-populated Metro Detroit — are now in “high” community levels, a CDC classification to show where COVID cases and hospitalizations have risen to the point that people are recommended to wear masks indoors. The city of Detroit is also at a high level, the city health department said.
Last week, only one county was considered to be at a high community level: Grand Traverse in the northern lower peninsula. Nearly every county spent most of April in the “low” category.
Another 28 counties are considered to be “medium” community levels, where people are advised to test for infections before socializing with those who may be more susceptible to severe COVID illness and to wear a mask around them. Those 28 counties account for another 30% of all Michiganians.
The results come after Michigan added 27,705 cases of COVID and 76 deaths from the virus on Wednesday, including totals from the previous six days. The state reported an average of about 3,958 cases per day over the seven days, a 46% increase from 2,706 cases per day last week and the fifth straight week cases have risen.
After declining for nearly three months, hospitalization rates in Michigan also increased for the fifth straight week.
“It’s concerning to see this after we got all the way down to low and got great numbers,” said Dr. Russel Faust, medical director of the Oakland County Health Division.
It is still early in the uptick to say what the results will be, experts say. But it appears fewer patients are getting dangerously sick, and for those who are sick, treatments exist.
“Hospitals have been getting better at managing this,” Faust said.
Dr. Matthew Sims, director of infectious disease research for Beaumont Health, said that upticks tend to follow a particular pattern. First, community levels rise, followed by a rise in hospitalizations, and then, a few weeks later, a rise in deaths. He estimated that if home tests were taken into consideration, the entire state would be in a high community level.
“We’re certainly not at a crisis point,” said Sims, acknowledging the number of COVID patients he has seen in recent days has risen. “But we could be there in a few weeks if things don’t go well. We’re going to keep watching this and doing everything we can.”
Case loads are better than they were in January, Faust said, when the first wave of the omicron variant rippled through the state and country. They’re worse than they were last summer, or even in March, but it seems so far that fewer people are getting seriously ill.
The downside of that is that “people have become more complacent,” Faust said.
“People who consider themselves more vulnerable, maybe because they’re older or they have other illnesses that would make them more susceptible, they’re still wearing masks,” he said. “But the majority of folks haven’t been wearing them, if you look around.”
That can help contribute to higher caseloads across Michigan. Masks are one of the most effective tools at limiting illness, he said, along with getting vaccinated, maintaining a safe distance from others and washing your hands properly for at least 20 seconds with soap.
“It’s the same old advice coming around again,” said Dr. Allison Weinmann, senior staff of infectious diseases at Henry Ford Health Systems, on Friday.
When people ditch their masks or aren’t fully boosted against COVID, more people are potentially exposed to illness. Even a person who is a while off from their doses may be at higher risk of catching or spreading the virus, Weinmann said.
Current CDC guidelines recommend that a person get both doses of a two-shot regimen and a first booster at least five months after that second shoot. Those 50 and older or who are immunocompromised can also get a second booster “at least four months after the first.”
There are also new variants coming through, substrains of the omicron variant. A new iteration of the omicron variant, BA.2, is now the dominant across Michigan and the country. Viruses like COVID have to evolve to keep infecting new patients, and it is the most infectious ones that become dominant strains.
“People may not necessarily be getting worse infections, but those particular variants are better at being transmitted than the last variant,” Faust said. “That’s what we’ve been watching happen around the world with past variants, and that’s what is happening with the omicron subvariants.”
That helps to explain why more counties are reaching high community levels not just in Michigan but around the country. More than 4% of all counties in the U.S. are at a high level this week, compared with 2.45% last week. More counties have also hit the medium level — 14.2% of counties are considered medium community levels, compared with just under 10% last week.
But even with an increase, Faust said the situation still isn’t as bad as it has been during previous case spikes.
“At this point, a lot of people are fully vaccinated and boosted or have been infected previously, which gives them a level of immune response,” he said. It is nearly impossible to say how many people would actually have a level of immunity against the newest strain, Weinmann said.
But any immunity can make a difference. People are still getting sick, but that immune response means that viral levels aren’t getting as high as they would if someone were exposed for the first time. That in turn means that most people aren’t getting severely sick.
“People still die from it. We need to make that clear: This is still not a cold or a flu,” Faust said. “But immunity across the community is way up, and that means our hospitals aren’t filling up and people are able to get the treatment they need.”
Weinmann said it is possible things could change. The current rise in cases is still relatively new. Every individual still needs to estimate their own risk levels, she said, adding it’s “never a mistake to wear a mask.”
“We’re going to be in this for the long haul. We’re going to see surges, and we have a fear that the next variant is going to be more transmissible and more deadly,” she said. “We’re not going to get out of this quickly, so now our goal needs to be: ‘How can I prevent myself and others from getting sick?’ That is still what we need to be thinking about.”
It is possible that even people who have been infected with recent variants may become infected again, Sims said. Research out of South Africa has shown that even people who were infected with BA.1, the original omicron variant, might not have the needed immunity to avoid getting sick from BA.4 and BA.5, the most recent omicron subvariants identified.
Sims said he felt it was probably time that the CDC expand the pool of people who can get a second booster in order to keep people as safe as possible. He pointed to bivalent vaccines, like the one Moderna has been working on, as the likely next step in vaccinations.
A bivalent vaccine is one that works against two different viruses (or, in the case of the new Moderna effort, multiple variants of the same virus). Many vaccines work that way, which is why flu shots change every year or why others, like pneumonia or HPV, have added additional strains over time.
Moderna’s new shot would target not only older COVID variants but also omicron variants specifically. The company said last month that initial results were promising, indicating that with additional research and federal approval, it could be used in the fall to protect against winter surges.
“We don’t have a magic bullet, some sort of medication that will save 90% of COVID patients, but we do have vaccines,” Sims said. “They are how you stay safe — you get vaccinated, you wear your mask in crowds, you protect yourself and everyone around you.”
Twitter: @Hayley__Harding