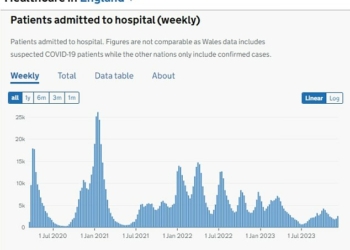
Shocking figures show more than 1.2 million people in the UK are estimated to have an eating disorder, and hospital admissions for those severely affected have risen by more than a third in recent years.
Meanwhile, Britain’s leading eating disorder charity, Beat, has reported an 80 per cent surge in calls to its helpline since the first Covid-19 lockdown in March last year.
As well as the emotional strain of the pandemic, the increase in figures is thought to be caused by a combination of factors — including the effect of social media on self-esteem and body image.

Britain’s leading eating disorder charity, Beat, has reported an 80 per cent surge in calls to its helpline since the first Covid-19 lockdown in March last year
But the question of why some people develop eating disorders in the first place has so far proved difficult to answer.
Three-quarters of those affected are women, who are thought to be more likely to experience negative perceptions of their body.
Known risk factors include having been criticised for your body shape, and having low self-esteem or an obsessive personality.
Another is having a family history of eating disorders. And now compelling new research shows the chances of developing major eating problems, such as anorexia nervosa, bulimia and binge eating disorder, could be much more heavily dependent on our genes than previously realised.
What’s more, the research suggests our genetic predisposition to being overweight or slim also dictates what type of eating problem we might experience.
For example, anorexia nervosa — where those affected starve themselves or exercise excessively — is much more common in those with ‘slim’ genes.
But those who are genetically more inclined to be overweight are more prone to bulimia and binge eating disorder, both of which involve gorging on food.

Known risk factors include having been criticised for your body shape, and having low self-esteem or an obsessive personality. Another is having a family history of eating disorders
The findings come from a team of researchers from the UK, U.S. and Switzerland, who studied the genetic profiles of more than 20,000 UK adults (just over 600 had eating disorders) to compare the DNA.
Previous studies had hinted that anorexia was more likely in those who are naturally slim. But it wasn’t clear if bulimia and binge eating disorder were more common in people genetically predisposed to being heavier.
As well as analysing DNA samples, scientists examined data on everything from volunteers’ weight to their history of mental health problems, such as depression, and if they had genes linked to obesity or slimness.
The team used this data to calculate the ‘polygenic risk score’ — an individual’s chance of developing certain illnesses compared to someone with a different genetic constitution.
The results, published recently in the International Journal of Eating Disorders, revealed those who had higher polygenic scores for anorexia tended to be already slim and had skinny genes, but those scoring highly for bulimia and binge eating disorder generally weighed more and had genes predisposing them to being heavier.
Researchers stress this does not mean being overweight alone increases the risk of bingeing-related disorders, or being slim means you will develop anorexia. Those risks only rise in people who also have a higher polygenic score for mental health problems.
The findings are another important piece in this jigsaw, says researcher Dr Christopher Huebel, from King’s College London.
‘We didn’t know those with bulimia or binge eating disorder are genetically more likely to weigh more. This means that if you have a high genetic liability to being fat, you have a higher risk of these disorders if you also have a greater genetic risk of mental illness.’
Dr Huebel adds that, in future, the findings may be used to identify youngsters most at risk of developing eating disorders.
Meanwhile, UK researchers are spearheading another major study, the Eating Disorders Genetics Initiative (EDGI), recruiting tens of thousands of people with eating disorders to provide saliva samples so we can better understand how genes might affect risk.
But some experts are unconvinced that genes are the main driver for eating disorders.
Dr Max Pemberton, a London-based NHS psychiatrist and Daily Mail columnist, says external influences, such as social media, are a much bigger problem.
He points to a landmark study on the Pacific Island of Fiji in the 1990s, when researchers from Harvard University scrutinised self-esteem and body image in a country where a fuller figure had traditionally been admired.
‘They didn’t find a single case on the island of anybody with an eating disorder,’ says Dr Pemberton.
‘Three years later, they found an increase in anorexia and bulimia. All that changed was the introduction of U.S. TV channels. Suddenly, the islanders were comparing themselves with each other and with skinny TV personalities.’
Dr Pemberton adds: ‘This latest genetic research is interesting and adds to our understanding of eating disorders. But it makes no difference to the way they are treated.’
To take part in the EDGI study, go to edgiuk.org