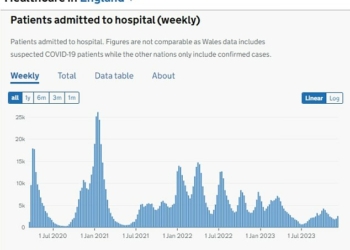
The Food and Drug Administration (FDA) has approved a new drug for HIV prevention that may be easier to take for many patients
This new drug, called Apretude, is taken by injection every two months. It could replace daily pills, which are challenging to take regularly and have a low uptake among some at-risk groups.
Clinical trials of Apretude found that one group of patients who took the injectable had a 69 percent lower risk of HIV infection compared to those who took daily pills, while a second group of patients had a 90 percent lower risk.
The new drug may be a great option for people at high risk of HIV, but potential patients could also face access barriers to the drug, which needs to be administered in a medical setting.
Existing preventative drugs for HIV are used disproportionately by white people, as opposed to the black and Hispanic or Latino Americans that make up a greater share of the high-risk population.

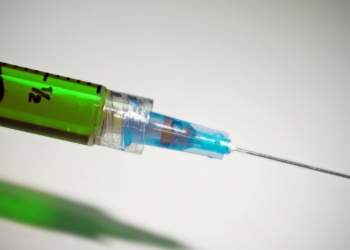
The FDA has approved a new preventative HIV drug, called Apretude, which is administered through injections. Pictured: A vial containing Apretude, provided by drugmaker Viiv

Existing HIV preventative medication is taken by a larger share of eligible white patients (orange bar) than black (green) and Hispanic/Latino (blue) patients, according to CDC data
While the COVID-19 pandemic has been at the forefront of healthcare in America for the past two years, the HIV/AIDS epidemic continues to impact thousands.
HIV (human immunodeficiency virus) attacks the body’s immune system. It can lead to AIDS (acquired immunodeficiency syndrome) if it isn’t treated.
The virus primarily impacts LGBTQ+ Americans, as well as black and Hispanic Americans.
Though HIV is treatable, the CDC recommends that people in at-risk groups take preventative measures to avoid infection in the first place.
On Monday, the FDA approved a new preventative drug for HIV that may be a better option for many of those people.
Patients receive this new drug, called Apretude, through an injection into the bloodstream once every two months.
Apretude was made by Viiv Healthcare, a pharmaceutical company based in North Carolina and owned by GlaxoSmithKline.
‘Today’s approval adds an important tool in the effort to end the HIV epidemic by providing the first option to prevent HIV that does not involve taking a daily pill,’ said Dr Debra Birnkrant, director of the Division of Antivirals in the FDA’s Center for Drug Evaluation and Research, in a statement.
‘This injection, given every two months, will be critical to addressing the HIV epidemic in the U.S., including helping high-risk individuals and certain groups where adherence to daily medication has been a major challenge or not a realistic option.’
The new drug may replace a daily pill regimen for many patients.
In 2020, only 25 percent of the 1.2 million people recommended to take PrEP pills were prescribed them, according to the CDC.
This is a major improvement from 2015, when only three percent of eligible Americans were prescribed the drug, but it’s still well below federal targets.
Existing PrEP usage is concentrated among white patients, even though the majority of patients eligible for the preventative pills are black and Hispanic or Latino.
About 66 percent of eligible white people were taking the pills in 2020, according to CDC data.
Meanwhile, only nine percent of eligible black people and 16 percent of Hispanic or Latino people who may benefit from PrEP received a prescription in 2020.

Research has shown that some groups at high risk of HIV face challenges in regularly taking daily pills, which were their primary option for prevention prior to the new drug approval. Pictured: Truvada, one of the pill options, shown in a French hospital in May 2012
CDC research has shown that some groups at high risk of HIV – such as young men who have sex with men – face significant challenges in regularly taking the daily pills.
At the same time, factors such as substance use disorders, depression, and poverty can impact patients’ ability to take their pills on schedule.
FDA scientists hope that the new drug, Apretude, may make it easier for patients to adhere to their treatment schedules.
‘People who are vulnerable to acquiring HIV, especially those in Black and Latinx communities who are disproportionately impacted in the US, may want options beyond daily oral pills,’ Deborah Waterhouse, the CEO of Viiv Healthcare, said in a statement.
‘That’s why ViiV Healthcare is proud that Apretude was studied in one of the most diverse and comprehensive HIV prevention trial programs to date, which also included some of the largest numbers of transgender women and Black men who have sex with men ever enrolled in an HIV prevention trial,’ Waterhouse said.
Viiv Healthcare tested the drug in two clinical trials, both of which compared patients who took Apretude injections every two months to patients who took a daily pill medication.
The first trial included about 4,600 cisgender men and transgender women who have sex with men.
In this trial, the patients who took Apretude had a 69 percent lower risk of HIV infection than the patients who took oral pills.
In the second trial, which included about 3,200 cisgender women, patients who took Apretude had a 90 percent lower risk of HIV infection than patients who took oral pills.

In clinical trials, patients who took the injectable treatment had lower risks of HIV infection than those who took pills: 69% lower in one trial and 90% lower in the other (file image)
Apretude’s side effects included injection site pain, headache, fever, fatigue, back pain, myalgia, and rash, the company reported.
The FDA warned potential patients that Apretude shouldn’t be used unless they have a negative HIV test, as a patient who has undiagnosed HIV before starting to use the drug may develop drug-resistant HIV.
The new drug may make it easier for millions of at-risk Americans to protect themselves from HIV infection.
But barriers to access may delay the treatment for many eligible people, Kenyon Farrow, managing director of the advocacy group PrEP4All, told NBC News.
‘Due to COVID, public health systems are already overburdened and much of the workforce needed to implement this large scale are leaving the field due to burnout,’ he told NBC in an email.
‘Because it will need to be administered in clinical settings, it won’t be treated as a pharmacy benefit by payers, but instead as a clinical benefit, which will take time to implement the proper coding for billing, as well as education and training for nurses who will likely bear the brunt of the work to implement.’