A prevailing theory as to how the omicron variant emerged so suddenly and jam-packed with mutations is that it was cultivated in an immune-compromised person — possibly someone with untreated HIV — with an extended coronavirus infection.
That proposal seems especially plausible to a team of scientists at Stanford, who treated a patient diagnosed with uncontrolled HIV and COVID earlier this year, and saw a striking development of mutations in the coronavirus over just 15 days.
The rise of omicron and the report from Stanford raise several key issues about the need to improve global COVID vaccination and ramp up HIV treatment at the same time to prevent the coronavirus from mutating further and prolonging the pandemic.
But there’s hope from the Stanford case: Both the HIV and the coronavirus infections were controlled by treating the patient with antiretroviral drugs. The woman is still HIV positive — there is no cure for HIV yet — but once that virus was suppressed by antiretroviral drugs and her immune system recovered, she quickly fended off the coronavirus with no ill consequences.
“If it is true that omicron came from an HIV-infected population, it does hit home that we cannot close our eyes to either of these pandemics,” said Dr. Jay Levy, an infectious disease expert at UCSF who was among the first to identify HIV as the virus that causes AIDS. “This is a wake-up call.”
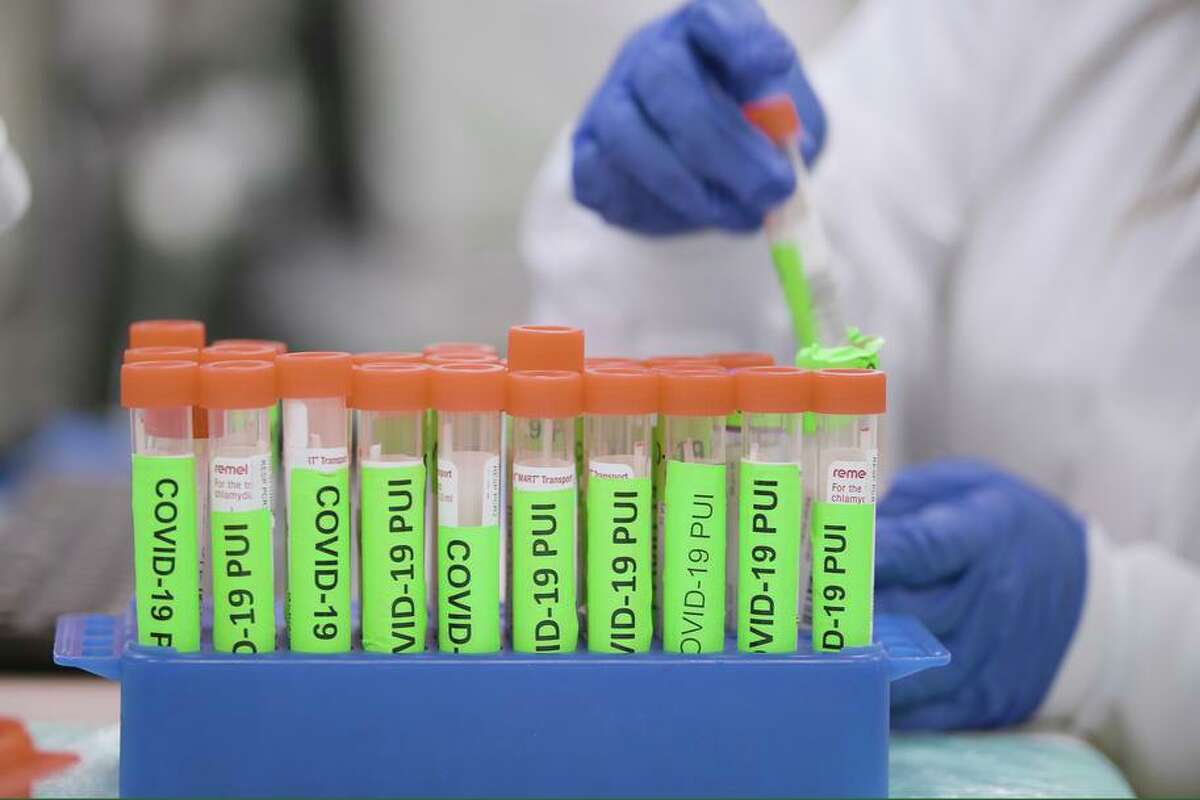
Coronavirus samples in the Stanford virology laboratory, where scientists are studying a possible link to HIV.
Stanford Medicine/Provided by Stanford Medicine
At the time the Stanford team treated the woman with HIV in January this year, a few examples of coronavirus variants had been reported as developing in immune-compromised patients, but none in patients with HIV. Some scientists have speculated that the alpha variant that sprang out of the United Kingdom last year emerged in a person undergoing treatment for cancer that included immune-suppressing chemotherapy, after they found specific mutations in one or more cancer patients with long-term COVID.
HIV is so dangerous because if left untreated it wipes out the immune system, leaving people vulnerable to all kinds of secondary infections, including many that are usually nonthreatening but can be deadly if the body can’t fend them off.
Drugs to treat HIV can’t get rid of the virus entirely, but they do a remarkable job of driving it to such low levels that people are otherwise healthy. In fact, HIV drug therapy aims to make the virus undetectable in the body, which preserves the health of individuals and also makes it next to impossible for them to infect others.
In the United States, and especially in the Bay Area, aggressive test-and-treat programs have resulted in the vast majority of people with HIV being diagnosed and treated quickly enough that their immune systems are never decimated and they don’t develop AIDS, the devastating syndrome that still kills roughly half a million people worldwide each year.
In other parts of the world — including southern Africa, where omicron is believed to have emerged — access to testing and treatment isn’t as widespread. That’s a public health dilemma on its own, but the confluence of unchecked HIV with widespread coronavirus transmission is especially problematic on a global scale, many experts say.
The main concern is over the emergence of new coronavirus variants with mutations that could make them more infectious, better at escaping the immune system or able to cause more severe disease than earlier strains. The threat that omicron poses remains uncertain at this point. But each new variant represents a potentially more dangerous foe in the pandemic.
The coronavirus develops mutations when it replicates, which occurs as it spreads from person to person, but also within the body of an individual. That means variants can emerge both from out-of-control spread of the virus in the community, but also in a single person who is infected for long enough that the virus accumulates multiple mutations.
Omicron has so many mutations — possibly as many as 50, including 32 on the spike protein that it uses to enter human cells — that many scientists have speculated it must have arose in one person with a lingering infection. It seems unlikely, they say, that a variant could spontaneously develop that many mutations just passing from one person to another.
“The explanation that (omicron) evolved over a long time and potentially in an immune-compromised person is probably right, because of that very sophisticated and complex accumulation of mutations,” said Dr. Warner Greene, a senior investigator at the Gladstone Institutes in San Francisco.
Evidence has already suggested that mutations can accumulate fairly rapidly if the virus is allowed to incubate in one person. And the Stanford case would seem to back that up too; the team published its formal report in October in Emerging Infectious Diseases, a journal from the U.S. Centers for Disease Control and Prevention.
The Stanford patient was a 61-year-old East Bay woman who was under 24-hour nursing care at home. She was already living with HIV, but not being treated for it, when she developed mild symptoms of COVID in mid-December 2020. She tested positive a few days after symptoms began, but never required hospitalization for COVID, and she had no symptoms by the time she was seen at Stanford in January.

A staff member at the Stanford Clinical Virology Laboratory works with COVID samples.
Steve Fisch/Stanford Medicine
She came to Stanford for treatment of a severe bedsore. At the time it was standard for all patients to be screened for COVID, and she tested positive again — now 30 days after she first reported symptoms, though she hadn’t felt ill for a couple of weeks. The Stanford test, which is somewhat more sensitive than the usual tests performed at most clinics, determined that she not only had the coronavirus in her nose, but that it was actively replicating.
Because she also had HIV that was not being treated, the woman’s immune system was in bad shape — her CD4 cells, a type of immune cell key to fighting infections that is notoriously destroyed by HIV, were almost nonexistent. The Stanford doctors started her on antiretroviral therapy for the HIV about a week into her hospitalization.
Within a month, her immune system had largely recovered and the amount of HIV in her blood was nearly undetectable. Meanwhile, less than two weeks after starting the HIV therapy, testing showed that the coronavirus was no longer actively replicating; about six weeks after that, she tested negative for COVID entirely.
“You’re actually attacking one pandemic, COVID, and the ongoing epidemic of HIV/AIDS, at the same time,” said Dr. Seth Hoffman, an infectious disease fellow at Stanford who treated the woman. “That’s really cool.”
Hoffman, recognizing that the woman was likely a rare case in the Bay Area — someone with untreated HIV who was co-infected with the coronavirus — asked colleagues if it would be useful to perform genomic sequencing on the coronavirus. Dr. Benjamin Pinsky, head of Stanford’s Clinical Virology Laboratory who had been ramping up sequencing of the virus since the start of the year, agreed.
They ended up sequencing two samples from the woman — one from the day she was admitted to Stanford and got her first nasal swab for testing, and a second 15 days later. In those two weeks, the virus developed at least five new mutations, including one that’s been associated with immune resistance in other variants. That mutation, in fact, is very similar to a mutation found in omicron.

Dr. Benjamin Pinsky, medical director of the Stanford Clinical Virology Laboratory, talks with a colleague in front of equipment used for genomic sequencing of the coronavirus.
Steve Fisch/Provided by Stanford Medicine
“Our patient only had three or four spike mutations” compared to the more than 30 with omicron, Pinsky said. “But they developed over the course of two weeks. You could easily imagine someone who is not on antiretrovirals who has HIV/AIDS, that they may have persistent levels of highly replicating (coronavirus) that could accumulate a large number of mutations.”
Infectious disease experts noted that in the Stanford case, because the woman was either under care at home or in the hospital during the course of her COVID illness, she never posed much risk to passing the mutated virus on to others.
The risk with variants is more serious in situations where immune-compromised people may be carrying the coronavirus for weeks or months and spreading mutated versions to others. Omicron may represent an example of that — the variant develops in one person, who then infects others in a climate of widespread community transmission that gives it plenty of room to become dominant.
The response, therefore, should be increasing overall vaccination to slow down spread of the coronavirus, but also treating HIV to prevent new variants from developing, Hoffman said. Omicron may be the strongest demonstration yet of the need to address COVID and HIV globally.
“The first case of omicron identified in the United States was in San Francisco, one of the wealthiest cities in the world,” Hoffman said. “If this came from an immuno-compromised person in southern Africa, or someplace else, that just speaks to the interconnectedness of our global community, and that we have to care about every member of our global community or we pay the price.”
Erin Allday is a San Francisco Chronicle staff writer. Email: eallday@sfchronicle.com Twitter: @erinallday