Marin County, where 90% of residents have been fully vaccinated against COVID-19, is California’s most vaccinated county.
During the current omicron surge, the county has, like others in the state, seen record-breaking case numbers. Hospitalizations, however, remain at a manageable level, and infected individuals who do require hospitalization are generally seeing shorter stays and not requiring intubation.
SFGATE talked to county Health Officer Dr. Matt Willis about the current surge, why omicron is so different from other variants and the future of pandemic policy. The interview has been lightly edited and condensed for clarity.
SFGATE: I wanted to follow up on something we discussed last week, where you said the general trend is that unvaccinated residents are more likely to wind up in the hospital than vaccinated residents, and the vaccinated residents who do end up hospitalized are “primarily older residents,” and that “even for that group it’s milder. They’re not on oxygen and not in the ICU as much as the past.” Is that trend holding?
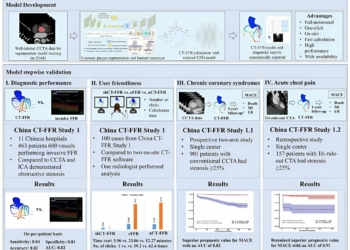
Willis: It is. All three hospitals are reporting an increase in the number of people coming into emergency departments with respiratory symptoms infected with COVID and omicron, but they are generally able to manage them and discharge them without sending them to ICU wards. In the past, we have distributed home oxygen kits, and there were criteria based on a patient’s oxygen level to determine if one needed. Right now, we’re not needing to distribute as many, and those who do require oxygen are requiring less oxygen than the past.
Fewer patients need intubation and breathing machines, which is consistent with other parts of world where omicron is the dominant variant they are seeing. Omicron tends to attack the upper airways and not the lower airways, when past strains were more aggressive in attacking sensitive tissue deep in the lung where oxygen is exchanged.
When people die of COVID, it’s usually due to respiratory distress and pneumonia, and we’re just not seeing as much of that pathology. The chest X-rays rays are more normal-looking.
SFGATE: Is the your county’s previous trend of “with COVID” and “for COVID” hospitalizations holding? Last time we talked, you said that at least eight of 19 patients listed as COVID-19 hospitalizations were incidental positives who in the hospital for other reasons.
Willis: The ratio is about the same, if not tilting more towards the “with COVID” side. For both groups, the numbers are increasing — yesterday we had 13 patients hospitalized “for COVID” and 12 hospitalized “with COVID” to make up 25 total, so it’s about half and half.
Each day, we receive communication from our hospitals with the distinction of two groups: “for COVID” and incidental positives. The way we’ve defined “incidental” is the simple of question of, “Would this person be in the hospital if they were not infected with COVID-19?” So mental health patients, obstetric patients and patients with other conditions, who, because the prevalence in the community is so high, we would expect to come in and test positive because every patient is tested upon entry.
SFGATE: When do you anticipate the current surge subsiding?
Willis: It’s hard to know. I think we’re looking at a combination of factors. Looking at the case rates themselves, that’s a less accurate indicator these days. Now, we we look at hospitalizations and waste water samplings. Waste water offers a real-time look at transmission. What we’re seeing from the waste water samples is that in some parts of the county, such as Novato, COVID is starting to plateau, but in some communities it’s still rising.
We do samplings twice a week and because things are changing so quickly, we would probably want to them daily. In terms of case rates, we’re at similar case rates today as we were one week ago, but it’s important to know that when we look at case rates, that’s based on PCR testing, which is in limited supply right now and more and more people are using home antigen that are not reported to public health. That’s why the waste water samples are increasingly important, because it offers a sense of the collective viral burden upstream, if you will.
It gives a sense of how much virus is present in the entire community, and Santa Clara just issued a statement saying they’re seeing a plateau in their waste water samples also, which is reassuring because across the Bay Area, the epidemiology has mostly been shared. As a region, we’ve traveled together through most stages of the pandemic; we’ve moved together on the timing and scale of waves we’ve experienced.
So when Santa Clara is seeing evidence of a plateau, that can be reassuring for the Bay Area as a whole, but it’s too early to tell.
SFGATE: You put out a video last week in which you say that once the current surge ends, we’re moving into a new phase where everyone will have to gauge their own individual tolerance for contracting COVID given risk levels. That seems to be pretty strong contrast from the previous two years where the number one imperative was reducing infections.
Willis: I do think that we have reached an inflection point in our response to this virus in terms of policies. That’s driven by a confidence in the strength of vaccine and the increasing evidence that if you’re vaccinated and infected, you almost always will have mild or no symptoms. Also, the omicron variant is so highly contagious it’s difficult to contain.
If our goal was preventing infections as it had been in past, we’d be reverting to lockdown policies as you’re seeing in some parts of world like China, Austria and Holland. While there are parts of the world seeking to prevent infections as the primary goal, we’re recognizing that policies that try to prevent all infections would lead towards greater societal harm than this version of virus will.
SFGATE: What’s the future of pandemic restrictions in Marin County? You haven’t closed businesses or banned gatherings, but are the Bay Area counties going to stick to the shared criteria for lifting the mask mandate, which includes a case-based criterion, after omicron ends? Which could lead to indefinite masking if case loads remain high given omicron’s transmissibility and the fact that you’re dealing with an endemic virus?
Willis: We will no longer be looking at case counts as an indicator for shifts in policy. For context, we estimate one in 20 residents are currently infected, so 5% of the county. Back-to-school testing kits gave us indicator of point prevalence, which is the percentage of the population that is infected right now. That’s hard to get, but because we did back-to-school testing among 38,000 people, we have a good estimate.
So the math is if you have any gathering of 100 people, we expect five to be actively infectious. So if you’re going to a movie or faith-based setting, you’re likely to have someone there spreading the virus. But we’re not reacting to that like we would have in the past, where public health policy would be to prevent such gatherings from occurring. Because results are more benign for vaccinated people, it’s up to individuals to understand the risk and make their own decisions based on risk tolerance and willingness to get infected.
Those at higher risk like people over 75 or people with serious conditions should think twice about going to certain high-risk settings, and should wear the best-quality mask like a K95. But from a policy standpoint, we’re not preventing that risk from occurring. When we had more virulent strains, it was our policy to halt transmission. I’m not questioning the need for those policies in the past, but it’s no longer as relevant for the current strain of the virus in a highly vaccinated area.
SFGATE: So on lifting the mask mandate specifically, you’d dump the case criterion?
Willis: Well some of this is where the laws lie. You’re talking to the county health officer, and legally, I can’t be less restrictive than the state. Right now, the state has an indoor mask mandate, so we’re following the state, which I think is appropriate. I agree with the need to cover our faces in indoor public settings right now. Lifting it is not my call, I can’t make that decision.
SFGATE: But once the state lifts it, if other Bay Area counties choose to keep the mandate until they satisfy the case criterion you all set, you’d break ranks?
Wills: We’d be looking at hospitalizations as our primary indicator, and importantly, hospitalizations “for COVID,” where it’s directly attributable to the virus. That’d be the primary metric we’d be looking to. We set a line to reimpose an indoor mask mandate at five hospitalizations per 100,000 residents. Right now, we’re at about six, so if there was no state mandate, we’d have issued our own, but we’re just slightly above that line.
SFGATE: There’s been reporting on the rise of “Vaxxed and Done” sentiments, where an increasing number of vaccinated residents believe the risk to them is akin to the flu or common cold, and want their 2019 lives back. Marin County is one of the most vaccinated counties in the country, where do you think your residents fall on this?
Willis: I think by and large it’s split down the middle. Some just want us to relax every policy and let it rip, and there are others who feel we’re being far too relaxed in what we’re already allowing. One of the ways we judge whether we’re being reasonable is if we get an equal amount of feedback from both ends of the spectrum, where is where we are now.
I think there’s a silent majority that’s walking that path with us, where each day we learn more and follow the best-available science to strike a balance between competing interests of mental, physical, social and economic health.
By and large our county has been responsive to the science and our vaccination rates are sign of that. People are aware that vaccinations are no longer protective against infection, and they’re not misunderstanding that the vaccine will magically protect them against testing positive. We’ve been very clear the primary benefit now is against severe illness.
It goes back to what I was saying about risk tolerance and individual choice. If you go into a movie theater where you know someone is probably infected, if you go into that encounter with your eyes wide open to the risk you’re assuming, that’s a more mature and sustainable way of relating to the virus. And that choice is offered by the protection the vaccine brings.
SFGATE: Do you think you’re having to hand-hold a lot of people out of pandemic mode and into endemic mode where, as you say, people will have assess risk and make their own choices?
Willis: Absolutely. One of primary challenges now is shifting our mindset. Our mental models and policies are based on a virus that was one thing in the past, and is something different now. It makes sense for our response to the virus to also change, but our experience of collective trauma over the past two years doesn’t get forgotten overnight.
We went through a period in Marin County where, even as a smaller county compared to the rest of the Bay Area, we had one death every two days. Now with vaccination, our mortality rates since May 2021 is on average just two deaths a month. One death every two days obviously leaves a mark.
Every case used to be cause for alarm, and there was a stigma tied up in that. All of that just needs to be put in rear-view mirror, and our way of approaching this virus needs to change. We’re dealing with a different variant of the virus; omicron does not behave like delta or alpha.
SFGATE: Because omicron is so different, one thing I’ve been wondering is what would happen if we actually did mass surveillance testing for the seasonal flu and common cold coronaviruses in previous years? If we actually went out and tried to find cases of those, would we see that the hospitalization and death rates are similar to omicron — especially in a highly vaccinated area like Marin and the Bay Area? Or even in areas with lower vaccination rates where lots of people are acquiring immunity now?
Willis: That’s a great question and a great way of framing this issue for the future. With influenza, we tolerated the consequences of influenza despite the fact that is led to 30,000 to 50,000 deaths a year. It has not occupied our societal dialogue, policies or tendencies. Public health tried to promote the flu vaccine for years, to limited success.
It’s a respiratory virus similar to SARS-CoV-2, where vulnerable populations are at risk, and ICUs during influenza are usually near capacity if it’s a bad flu season. Being able to place COVID alongside other known viral threats will be important. There’s also respiratory syncytial virus, or RSV, which causes younger children to have trouble breathing. RSV is a much bigger threat for children than COVID. We saw way more hospitalizations for children with RSV in years past than we saw for children with COVID since the start of the pandemic. RSV never changed public policy and behaviors.
SFGATE: What do you think life in Marin County will look like six or seven months from now? It’s late summer, school will be about to restart for new year, is everything back to normal and looking like 2019? Could COVID-19 be out of mind?
Willis: I think the answer to that question is dependent on what variants we are seeing at that time. It’s likely SARS-CoV-2 will continue to evolve, and there will be new variants. Omicron has demonstrated how radically this virus can develop mutations. It would be a mistake to assume this wouldn’t happen again just because of the biology, and we haven’t suppressed the virus in most parts of the world yet because of a lack of access to vaccines.
I do feel reassured about subsequent variants being less virulent because it’s just the way viruses tend to evolve, and omicron is an example of that. We have the tools to respond, especially vaccines. My hope is if we do see another wave, what’s promised by the federal government in terms of treatment will come and we’re all prepared. I think we’ll be prepared not just on the infrastructure but also on the biology, because in our area, we have access to vaccines, and after omicron moves through we’ll have another added layer of protection from natural immunity after being infected, which means the next wave would be likely milder for us.
It’s hard to predict. We can’t know whether we’re going to face another wave or not. But we know the basic principles that will apply across any wave, and we know to be responsive to the particulars of a variant when it occurs and be flexible. If it’s more virulent, we may have to resort to more restrictive policies
SFGATE: As I understand, a “doomsday variant” that is more virulent and evades’ vaccine protection against severe disease is highly, highly unlikely. Like you said, viruses tend to grow less virulent over time?
Willis: Very unlikely. The smartest viruses like colds have learned to coexist peacefully with the human population because they don’t make you so sick that you can’t move about the community and infect others. So that’s a powerful driver of evolution, and omicron is the perfect example of this.
Omicron is showing how successful it is at copying itself across the population by not making people very ill and being extremely contagious. I expect future variants will be similar, but it’s all probability. Fortunately, something more virulent is very unlikely.