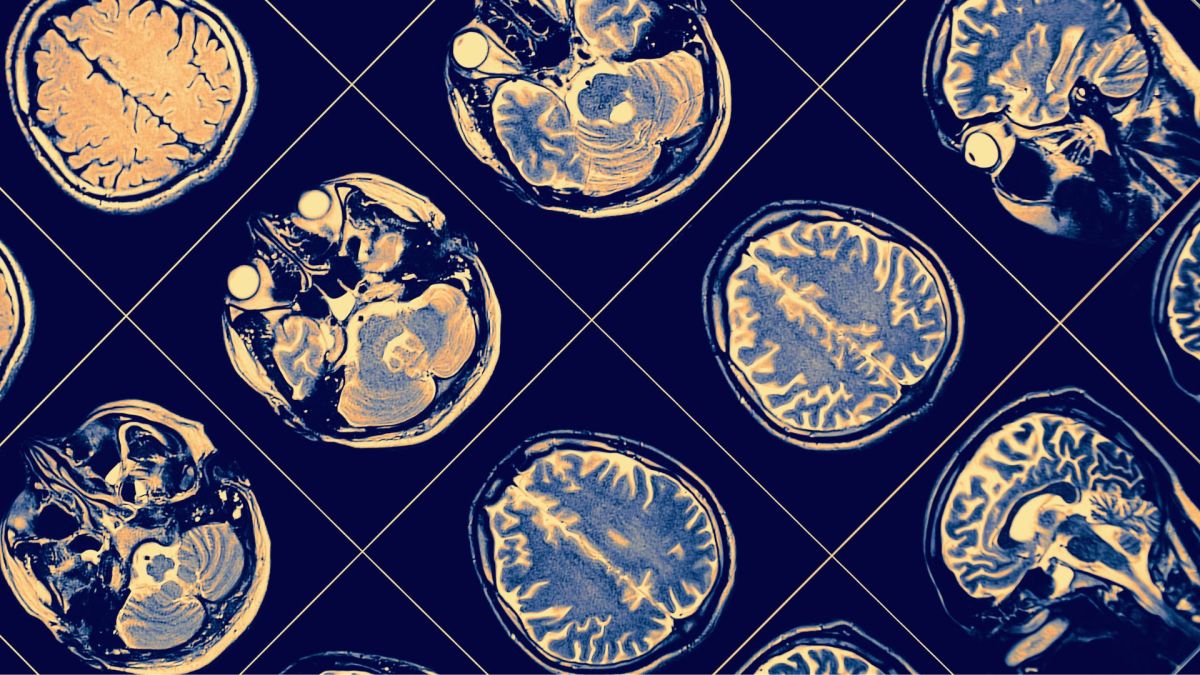
The brains of older adults with obesity show patterns of gray matter loss that are strikingly similar to those seen in people with early Alzheimer’s disease, a new study suggests. These patterns overlap in the location of the tissue loss but not in the severity; in other words, Alzheimer’s patients exhibit a far greater degree of brain atrophy than cognitively healthy, obese adults of the same age do.
“The degree of the changes is much lower in obesity,” confirmed Filip Morys (opens in new tab), first author of the new study and a postdoctoral fellow at McGill University’s Montreal Neurological Institute. However, the spatial distribution of the tissue loss may help to explain why obesity is a major risk factor for Alzheimer’s, Morys told Live Science; past studies have specifically linked midlife obesity to an increased risk of Alzheimer’s and other types of dementia down the line.
“It’s further evidence that this major cardiovascular risk factor of obesity is linked with evidence of neurodegeneration,” or the progressive loss of brain cells, said Dr. Jeffrey Burns (opens in new tab), co-director of the Alzheimer’s Disease Research Center at the University of Kansas Medical Center, who was not involved in the study.
However, the new research, published Tuesday (Jan. 31) in the Journal of Alzheimer’s Disease (opens in new tab), cannot reveal the exact cause of this tissue loss, nor can it pinpoint which of the cognitively healthy, obese participants might go on to develop dementia, Burns told Live Science. That’s partly because the analyses captured only one point in time, in each participant’s early to mid-70s.
Related: New Alzheimer’s drug slightly slows cognitive decline. Experts say it’s not a silver bullet.
“We need long-term, longitudinal studies where we’re measuring these things over time,” Burns said. “For these individuals without cognitive issues, how strongly is this linked to poor outcomes in the future?” We don’t know yet.
Prior to their new study, Morys and his colleagues found evidence that, in people in their 60s, obesity seems linked to distinct patterns of thinning in the brain’s gray matter. Named for its color, gray matter is made up of the bodies of brain cells, or neurons, and the uninsulated wiring that extends from those cells; gray matter is found primarily in the cerebral cortex, the brain’s wrinkled outer surface.
“We saw that the patterns there are very similar to the ones we see in Alzheimer’s disease,” Morys said of that previous work, published in 2021 in The Journal of Clinical Endocrinology and Metabolism (opens in new tab). To further investigate these similarities, the team tapped two huge databases of brain scans: the Alzheimer’s Disease Neuroimaging Initiative (ADNI) database and the UK Biobank.
From the ADNI database, which was compiled in the U.S., the team pulled brain scans from people diagnosed with mild Alzheimer’s and from healthy individuals without any cognitive impairment. From the UK Biobank, they compiled brain scans from cognitively healthy individuals and grouped them by body mass index (BMI), a measure used to estimate excess body fat.
In all, the team used brain scans from more than 1,300 individuals to generate maps of cortical thickness for people of different BMIs and people with and without Alzheimer’s. By comparing the maps, they pinpointed regions of the cortex that appeared thin in people with obesity and those with Alzheimer’s, but not in lean, cognitively healthy individuals. These overlapping regions showed up even when people with both obesity and Alzheimer’s were excluded from the analysis.
“This study demonstrates that areas of cortical thinning seen in lean persons with AD [Alzheimer’s disease] are the same areas that are thin in those with obesity,” Dr. Heather Ferris (opens in new tab), an assistant professor of endocrinology and metabolism and neuroscience at the University of Virginia (UVA) Health who was not involved in the study, told Live Science in an email.
These thinned-out regions included the right temporo-parietal cortex and left prefrontal cortex, which are involved in high-level cognitive functions, such as long-term memory, language, attention and executive functioning, or the ability to plan and execute tasks, Morys said. “If you look at patients with AD, [problems with these functions] are often the first signs of the disease,” he added.
But again, as this study offered only a snapshot in time, the researchers cannot predict if any of the cognitively healthy, obese participants will go on to develop dementia, Morys said. And the team cannot conclusively say what caused these individuals’ gray matter to thin in the first place.
Conditions that often occur in obesity — such as systemic inflammation, high blood pressure and type 2 diabetes — can potentially injure brain cells and have been linked to Alzheimer’s-related brain changes, the researchers wrote in their report. That said, there may be brain-thinning mechanisms at play in obesity that are totally independent of those seen in Alzheimer’s, the team wrote.
In the future, Morys and his colleagues aim to conduct a large clinical trial to see if weight loss treatments can guard against later cortical thinning and cognitive decline. On that front, there’s a huge question as to when such interventions should be started, Ferris said.
“While many of the effects of obesity are reversed with weight loss, once a neuron has died it is gone and [is] not going to be replaced,” Ferris said. “That means that if weight loss will lower the risk of AD, it likely needs to occur before significant brain loss occurs. When that is can’t be answered by this study.”