Summary: Stress, anxiety, and depression during pregnancy were associated with altered key features in fetal brain development, resulting in decreased cognitive offspring in a child at 18 months of age.
Source: Children’s National Hospital
Women’s elevated anxiety, depression and stress during pregnancy altered key features of the fetal brain, which subsequently decreased their offspring’s cognitive development at 18 months.
These changes also increased internalizing and dysregulation behaviors, according to a new study by Children’s National Hospital published in JAMA Network Open. Researchers followed a cohort of 97 pregnant women and their babies.
The findings further suggest that persistent psychological distress after the baby is born may influence the parent-child interaction and infant self-regulation.
This is the first study to shed light on an important link between altered in-utero fetal brain development and the long-term cognitive development consequences for fetuses exposed to high levels of toxic stress during pregnancy.
While in the womb, the researchers observed changes in the sulcal depth and left hippocampal volume, which could explain the neurodevelopment issues seen after birth.
Once they grow into toddlers, these children may experience persistent social-emotional problems and have difficulty establishing positive relationships with others, including their mothers. To further confirm this, future studies with a larger sample size that reflect more regions and populations are needed.
“By identifying the pregnant women with elevated levels of psychological distress, clinicians could recognize those babies who are at risk for later neurodevelopmental impairment and might benefit from early, targeted interventions,” said Catherine Limperopoulos, Ph.D., chief and director of the Developing Brain Institute at Children’s National and senior author of the study.
Regardless of their socioeconomic status, about one of every four pregnant women suffers from stress-related symptoms, the most common pregnancy complication. The relationship between altered fetal brain development, prenatal maternal psychological distress and long-term neurodevelopmental outcomes remain unknown.
Studying in utero fetal brain development poses challenges due to fetal and maternal movements, imaging technology, signal-to-noise ratio issues and changes in brain growth.
All pregnant participants were healthy, most had some level of education and were employed. To quantify prenatal maternal stress, anxiety and depression, the researchers used validated self-reported questionnaires.


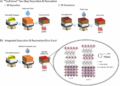
Fetal brain volumes and cortical folding were measured from three-dimensional reconstructed images derived from MRI scans. Fetal brain creatine and choline were quantified using proton magnetic resonance spectroscopy. The 18-month child neurodevelopment was measured using validated scales and assessments.
This study builds upon previous work from the Developing Brain Institute led by Limperopoulos, which discovered that anxiety in pregnant women appears to affect the brain development of their babies. Her team also found that maternal mental health, even for women with high socioeconomic status, alters the structure and biochemistry of the developing fetal brain. The growing evidence underscores the importance of mental health support for pregnant women.
“We’re looking at shifting the health care paradigm and adopting these changes more broadly to better support moms,” said Limperopoulos.
“What’s clear is early interventions could help moms reduce their stress, which can positively impact their symptoms and thereby their baby long after birth.”
About this psychology and neurodevelopment research news
Author: Press Office
Source: Children’s National Hospital
Contact: Press Office – Children’s National Hospital
Image: The image is in the public domain
Original Research: Open access.
“Association of Elevated Maternal Psychological Distress, Altered Fetal Brain, and Offspring Cognitive and Social-Emotional Outcomes at 18 Months” by Catherine Limperopoulos et al. JAMA Network Open
Abstract
Association of Elevated Maternal Psychological Distress, Altered Fetal Brain, and Offspring Cognitive and Social-Emotional Outcomes at 18 Months
Importance
Prenatal maternal psychological distress is associated with disturbances in fetal brain development. However, the association between altered fetal brain development, prenatal maternal psychological distress, and long-term neurodevelopmental outcomes is unknown.
Objective
To determine the association of fetal brain development using 3-dimensional magnetic resonance imaging (MRI) volumes, cortical folding, and metabolites in the setting of maternal psychological distress with infant 18-month neurodevelopment.
Design, Setting, and Participants
Healthy mother-infant dyads were prospectively recruited into a longitudinal observational cohort study from January 2016 to October 2020 at Children’s National Hospital in Washington, DC. Data analysis was performed from January 2016 to July 2021.
Exposures
Prenatal maternal stress, anxiety, and depression.
Main Outcomes and Measures
Prenatal maternal stress, anxiety, and depression were measured using validated self-report questionnaires. Fetal brain volumes and cortical folding were measured from 3-dimensional, reconstructed T2-weighted MRI scans. Fetal brain creatine and choline were quantified using proton magnetic resonance spectroscopy. Infant neurodevelopment at 18 months was measured using Bayley Scales of Infant and Toddler Development III and Infant-Toddler Social and Emotional Assessment. The parenting stress in the parent-child dyad was measured using the Parenting Stress Index-Short Form at 18-month testing.
Results
The cohort consisted of 97 mother-infant dyads (mean [SD] maternal age, 34.79 [5.64] years) who underwent 184 fetal MRI visits (87 participants with 2 fetal studies each) with maternal psychological distress measures between 24 and 40 gestational weeks and completed follow-up infant neurodevelopmental testing.
Prenatal maternal stress was negatively associated with infant cognitive performance (β = −0.51; 95% CI, −0.92 to −0.09; P = .01), and this association was mediated by fetal left hippocampal volume. In addition, prenatal maternal anxiety, stress, and depression were positively associated with all parenting stress measures at 18-month testing.
Finally, fetal cortical local gyrification index and sulcal depth were negatively associated with infant social-emotional performance (local gyrification index: β = −54.62; 95% CI, −85.05 to −24.19; P < .001; sulcal depth: β = −14.22; 95% CI, −23.59 to −4.85; P = .002) and competence scores (local gyrification index: β = −24.01; 95% CI, −40.34 to −7.69; P = .003; sulcal depth: β = −7.53; 95% CI, −11.73 to −3.32; P < .001).
Conclusions and Relevance
In this cohort study of 97 mother-infant dyads, fetal cortical local gyrification index and sulcal depth were associated with infant 18-month social-emotional and competence outcomes, and fetal left hippocampal volume mediated the association between prenatal maternal stress and infant cognitive outcome.
These findings suggest that altered prenatal brain development in the setting of elevated maternal distress has adverse infant sociocognitive outcomes, and identifying early biomarkers associated with long-term neurodevelopment may assist in early targeted interventions.